Apply the Evidence to the Desired Clinical Situation
If you have located quality evidence to use in clinical decision making, you must determine if the evidence is generalizable to your patient, feasible in your situation, and matches your patient’s expectations. Establishing the generalizability of a study centers around how similar your patient is to the participants in the study. Your patient is more likely to respond according to the study if he or she is a member of that population. Consider age, gender, level of competition/experience, length of injury/recovery, and prior injuries. Next, is the treatment feasible in your facility and with your level of experience? Be sure that your interest in trying a new technique is not overshadowing some practical issues. Do you have the same equipment? Can you provide the same frequency and duration of treatments? Are you knowledgeable enough to perform the treatment or test? If not, are there ways for you to learn more or practice in advance? Finally, do the potential benefits outweigh the potential harms for the patient?
EBP provides a 3-pronged approach to patient-centered care. Such as with the legs of stool, all prongs are equally weighted (Figure 5-3). The first leg is using the best available evidence in decision making. Leg 2 takes advantage of the clinician’s expertise and experience to provide the highest quality care. The third leg supports the patient’s needs and preferences about his or her care. Ask yourself if this treatment is suitable for this patient. Consult with your patient and involve him or her in the final decision before implementing the treatment.
If the patient’s preferences and values are not taken into consideration, patient compliance, persistence, and follow-through may be lacking, and the treatment will lose a measure of effectiveness. For example, if the patient finds that the core strengthening program you prescribed for his or her back injury is too difficult, time consuming, or complicated, his or her compliance will suffer, and the potential for a positive outcome is reduced. There are many issues to discuss with patients, such as the following:
• Their outcome goals and expectations
• What support they have from family and friends and whether their family and friends have to help with the treatment (eg, transportation, self-care, or encouragement)
• Whether the proposed treatment is in line with their religious, moral, cultural, or ethical beliefs
• How rigorous, complicated, or time demanding the treatment be will
• The potential side effects or less-than-ideal outcomes
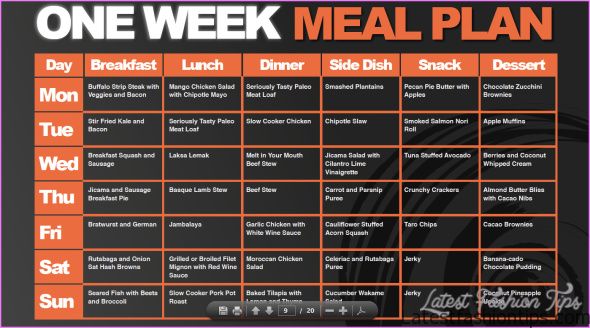
Meal Plan And Exercise Plans For Weight Loss Photo Gallery
• Whether the financial costs of the treatment (missed work, medical bills) will create hardship. One commonly used method for creating a usable document that summarizes and stores evidence and the clinical bottom line is a critically appraised topic (CAT). The CEBM4 provides a method for writing CATs (www.cebm.net/catmaker-ebm-calculators/). Clinicians can also locate CATs in various professional journals (ie, Journal of Sports Rehabilitation). CATs are typically limited to 2-page document that include a summary of the search process and results. It also includes a summary table of the articles that were appraised.4 The components of the CAT include, but are not limited to, the following:
• Focused clinical question (PICO)
• Search strategy (terms used, databases; inclusion/exclusion criteria)
• Summary of the findings (number of articles, types of research articles)
• Best evidence (summary of level of evidence)
• Best evidence/key findings (summary of key points, similarities, or differences in articles)
• Clinical bottom line (based on key findings; what you will apply).
Step 5: Evaluate the Efficacy and Efficiency of the Practice
Well-defined, objective measures should be used to determine the clinical benefit of the treatment and the patient’s experience. Clinically oriented outcomes include measures of pain, range of motion, strength, and scores on functional tests. Patient-oriented outcome measures relate to meeting patient goals and expectations and may include return to work or play, ratings of satisfaction with the treatment, and perceived benefits. Clinical measures should be taken prior to treatment, every few sessions thereafter, and at the end of the treatment plan. Patient-oriented measures typically occur after the last session and may be done less formally through conversation. Review the data and assess how well the treatment worked. This is also the time to determine if there are any factors that helped or hurt the outcome. These factors become new evidence to be used in the future.
When beginning to perform regular searches on clinical questions, it is also important to catalog and periodically update the searches as more evidence becomes available. At first, this step appears to be very time consuming, but establishing a regular day and time allotment helps. The goal is not to answer every question you have, but to seek new ideas and stay involved in the literature. You can engage colleagues by sharing your questions and results. The following questions will help guide you:
Are you consistently asking and following through on your clinical questions?
What questions or interesting ideas have presented themselves recently in your practice?
Maybe You Like Them Too
- Tamar Braxton A Life in Music
- Sunny Hostin A Biography
- Steve Coogan A Life in Comedy
- Sterling K Brown A Biography
- Stephen A. Smith A Biography